Now with BABY DOPPLER
Never miss the heartbeat
Shop Fetal Dopplers from the Most Trusted Seller of Heart Monitoring Devices
Best Sellers

DuoSmart Ear & Forehead Thermometer for Baby/Child/Adult - FDA Approved
was USD $89.95 Special Price USD $12.97

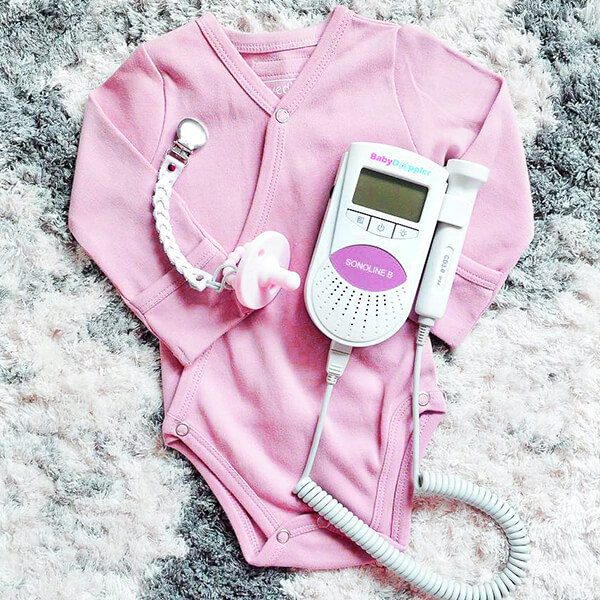
The Official BabyDoppler® Sonoline B Fetal Doppler (Pink)
was USD $69.95 Special Price USD $49.95

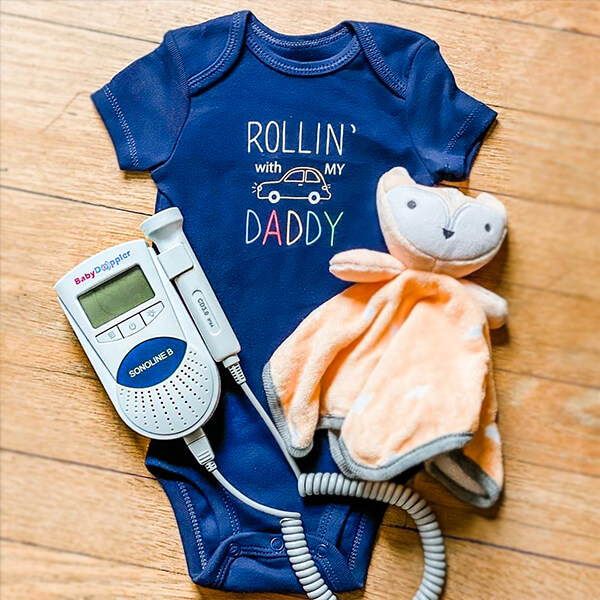
The Official BabyDoppler® Sonoline B Fetal Doppler (Blue)
was USD $69.95 Special Price USD $49.95

The Official BabyDoppler® Sonoline B Fetal Doppler (Teal)
was USD $69.95 Special Price USD $49.95
What our Customers have to say




















Instagram @babydoppler


- 11 0
I am changing my name to Mom! When is your due date? Comment below and let us know! 💕 #repost via b...
- 9 3
Ghouls just want to have some fun. Isn't? How adorable is this spooky snack 🍪❤️ #repost via @k...
- 9 0
Who is expecting their little bundle of joy this month? Comment down and find your due date buddy! 💕...
- 12 0
No tricks, just treats! ❤️ #repost via @themagicplaybook #babydoppler #halloween #halloweenishere ...
- 12 0
Roses are red, violets are blue, counting down the days until we meet you our little boy!❤️ #repost...
- 7 0
"Taking my families temperature has been part of our routine for a while. Thanks to Baby Dopple...
- 22 3
Hello Moms! Who is expecting their little bundle of joy this month? Comment down and find your due d...
- 13 0
You're my pumpkin pumpkin.. .. 🎃🥰 #repost via @madnatorr #babydoppler #pumpkinbaby #babystyle...
- 10 0
"One of my pregnancy must haves! Our baby Doppler has been so precious to us this pregnancy, we...
- 12 0
Roses are red, violets are blue, counting down the days until we meet you! Were you excited for you ...
- 14 0
Life’s biggest miracle is the gift of having life growing inside of you!💕 #repost via lemons.for.da...
- 3 0
Falling leaves and falling prices. Fall in love all over again with Baby Doppler’s flash sale discou...